CBT Cognitive Behavioural Therapy (CBT) is a psychotherapeutic approach which is used to treat a range of emotional difficulties, as well as the psychological impact of physical health problems.
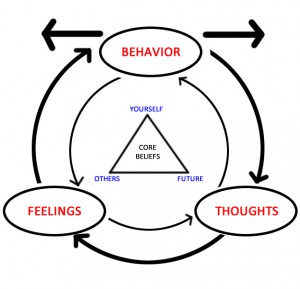
The CBT approach provides a model for understanding the relationships between our thoughts, feelings, behaviour or actions and how we physically feel within ourselves. Different CBT models have been developed for working with different issues or difficulties, but generally the approach focuses on developing a deeper understanding of the thought patterns and behaviours maintaining a problem. Cognitive Behaviour Therapy can be used to treat a range of conditions (please see treatment section for further information).
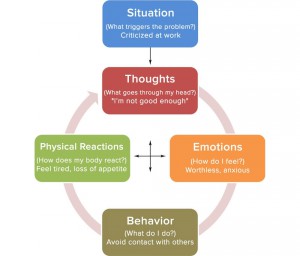
Direct work with the individual includes assessment of their thoughts, behaviours, feelings and physical sensations, and how they interrelate.
From this initial assessment a therapeutic plan is developed, to help them to overcome the problem or difficulty with which they’re struggling.
Cognitive Behavioral Therapy (CBT) is a form of psychotherapy that focuses on our thought patterns, and how our thinking can affect our behaviour, and how we feel overall. The aim of CBT is to teach you new ways of thinking in order to help you change a certain behaviour, or to find a more positive perspective on a particular issue. According to CBT, changing how we think about and approach a challenge can help us deal with it more effectively, thereby improving our own situations.
CBT was originally conceived of as a way to treat depression. The logic behind this was quite simple: if you think negative, you feel negative. When the therapy was first tested, it was hoped that it could be used to treat depression by helping people focus on the positive aspects of their lives. Years later, it is now widely accepted that CBT can be just as if not more effective than medication in treating depression, and can have much more long-term effects. This is due to the fact that reframing out thought processes is essentially a skill we learn, and every time we apply it to a situation, we become more skilled at it.
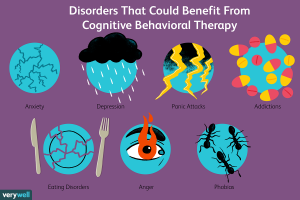
The results of CBT in treating depression have been so positive that it is now used to treat a wide range of conditions, such as post-traumatic stress disorder, phobias, anger issues, substance abuse, eating disorders, and much more. Both in theory and in practice, CBT can be applied to any maladaptive behavior that is triggered by or in response to our thought processes.
Eating disorders are a good example of a problem that runs rampant throughout western civilisation, but can benefit greatly from CBT. Countless studies have linked the rise in Anorexia Nervosa directly to Western culture and media, where images of unrealistic beauty standards are highlighted in a near-constant basis. This leads more and more people towards the maladaptive behaviour of allowing themselves to go hungry, rather than risking any weight gain.

CBT can help with conditions like this by helping the patient to see these images in a very different way. By walking a patient through the real numbers of how many people actually look like the models we see, the negative health effects of techniques used to achieve those looks (unhealthy diets, smoking, plastic surgery), the use of professional makeup artists alongside digital manipulation, a therapist can begin to help a patient reframe their thinking. The goal is that by the end of the therapy, a patient who sees these images will not begin to think about their own physical flaws, but will instead think about the amount of work and trickery that goes into creating these unrealistic images.
